Vanderbilt-Ingram Cancer Center names co-leaders for Thoracic Oncology Program

Vanderbilt-Ingram Cancer Center has named Fabien Maldonado, MD, MSc, and Evan Osmundson, MD, PhD, as co-leaders of its Thoracic Oncology Program, reflecting the center’s commitment to expanding disease-specific cancer care for patients across the region.

As co-leaders, Maldonado and Osmundson will identify gaps and opportunities to improve prevention, detection and treatment of lung cancer. They will build collaborative bridges across thoracic specialties — including thoracic surgery, pulmonology, radiology, pathology, and medical and radiation oncology — recognizing that lung cancer treatment frequently requires a coordinated, multimodal approach.
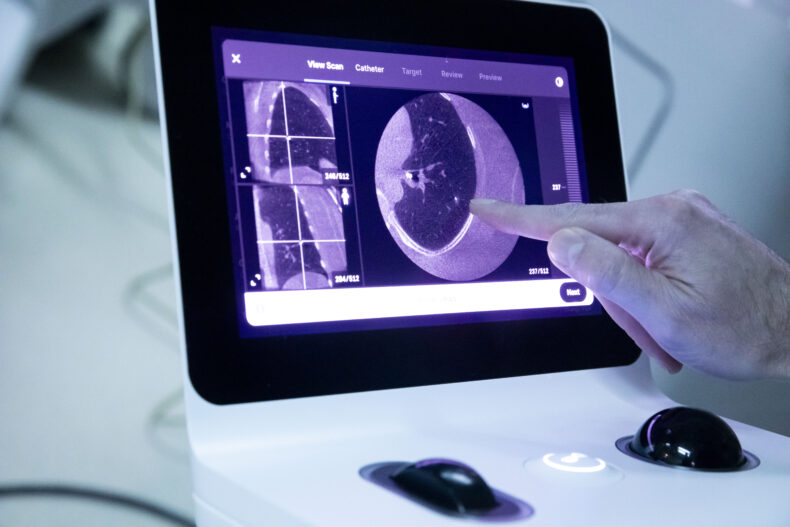
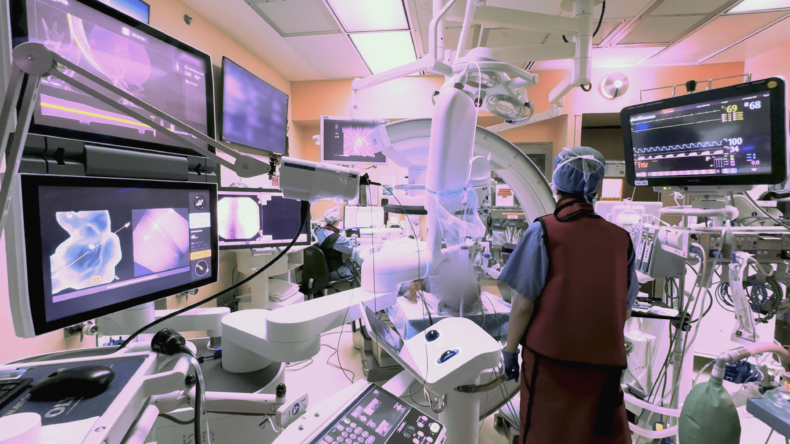
They will also work to expand access to innovative technologies, including robotic bronchoscopy, which enables biopsy of previously unreachable areas of the lung; advanced local therapies such as minimally invasive surgery and adaptive radiotherapy; and targeted systemic treatments tailored to each patient’s tumor. This work will reduce wait times, improve diagnostic accuracy, lower toxicity and deliver personalized therapy within a multidisciplinary, team-based model of care.
“Lung cancer is a top priority for our cancer center because Tennessee has among the highest rates of lung cancer mortality in the country,” said Ben Ho Park, MD, PhD, the Benjamin F. Byrd Jr. Professor of Oncology and Director of Vanderbilt-Ingram. “The number of Tennesseans who smoke is higher than the national average, and our screening rates are lower — a combination that disproportionately affects our communities. The best way to cure lung cancer is to catch it early. Under the leadership of Drs. Maldonado and Osmundson, we are rebooting our Thoracic Oncology Program to bring together lung cancer researchers, care providers and trainees across Vanderbilt-Ingram in an even more collaborative way. That collaboration will drive higher-impact research and discoveries that translate quickly into meaningful benefit for our patients and the people of Tennessee.”
Maldonado, Professor of Medicine, Thoracic Surgery and Mechanical Engineering, focuses his research on clinical trials in interventional pulmonology, CT-based quantitative imaging for lung cancer and robotic bronchoscopy.
“Major advances in lung cancer care, including lung cancer screening and minimally invasive diagnostic and therapeutic interventions, have improved lung cancer survival rates by more than 25% over the past five years; however, much work remains, and we are excited to continue building the most patient-centered, data-driven, and technologically advanced lung cancer program in the state of Tennessee,” said Maldonado, who holds the Pierre Massion Directorship in Lung Cancer Research.
Osmundson, Associate Professor and Vice Chair of Clinical Operations in the Department of Radiation Oncology, where he serves as medical director, is board-certified in radiation oncology. He specializes in thoracic malignancies and lymphoma and leads several investigator-initiated clinical trials designed to enhance the synergy between radiation therapy and immunotherapy, with funding from the National Institutes of Health and other entities. He has also become a leading voice for patients facing barriers to care, with research advocating for prior authorization reform to reduce treatment delays in oncology.
“Thoracic oncology has entered a remarkable era of personalized medicine, in which therapies tailored to each patient’s individual cancer are producing outcomes we couldn’t have imagined even a decade ago. Patients are living longer and, importantly, living better than ever before, yet we know there’s still much further to go,” said Osmundson. “At Vanderbilt, our innovative research and clinical programs have helped drive this revolution, and our team-based care brings these discoveries to patients today. I’m more excited than ever to extend this care across our region and to discover what comes next.”
Together, the co-leaders bring complementary expertise aimed at delivering the most innovative and advanced options for patients at all stages of lung and other thoracic cancers. The goal of the Thoracic Oncology Program is to improve survival and quality of life — personalizing treatment for every patient, regardless of when they arrive at Vanderbilt-Ingram.
The post Vanderbilt-Ingram Cancer Center names co-leaders for Thoracic Oncology Program appeared first on Vanderbilt Health News.